
(f) Deploying a bioresorbable polymer sirolimus-eluting stent (Ultimaster® 3.0 ∗38 mm). Intravascular ultrasound (IVUS) images at the culprit lesion (i) and at the coronary ostium (ii). (e) Angiogram after dilatation with a 2.5 mm semicompliance balloon.
#Guideliner manual
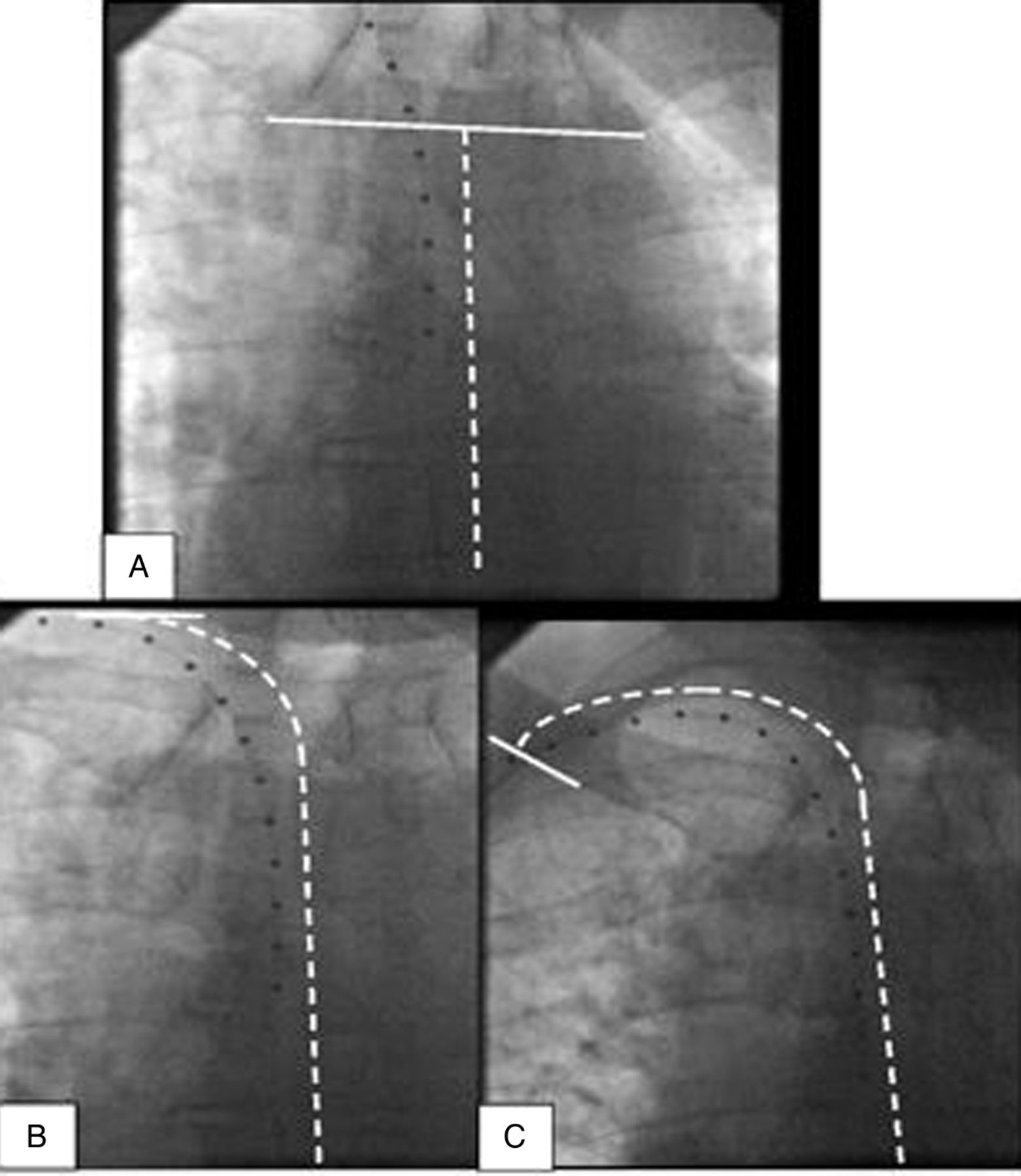
In order to avoid coronary dissection, the contrast medium was gently introduced via manual injection. (d) After anchoring it with a 1.5 mm balloon, the GuideLiner catheter was selectively introduced into the left coronary artery. (c) A 1.5 mm semicompliance balloon in the lead, along with a mother-child system, including a 6-Fr AL-1 guide catheter and a GuideLiner catheter, was advanced close to the orifice of the coronary trunk. (b) Removing the 5-Fr diagnostic catheter, leaving only the guide wire. We then engaged the coronary trunk by using a 5-Fr diagnostic catheter, and a 0.014-inch guide wire was advanced across the LAD lesion. (a) We failed to engage the coronary trunk by using a 6-Fr AL-1 guiding catheter.

During the procedure, the volume of contrast medium used was 75 mL, and the radiation exposure dose was 0.78 Gy. A final angiogram showed adequate and favorable dilatation of the culprit lesion ( Figure 2(g)). The stent was additionally dilated with a noncompliance balloon 3.5 ∗12 mm ( Figure 2(g)). In order to avoid coronary dissection, contrast medium was gently injected using a manual method.After dilatation with a 2.5 mm semicompliance balloon ( Figure 2(e)), we have implanted the bioresorbable polymer sirolimus-eluting stent (Ultimaster 3.0 ∗38 mm, TERUMO, Tokyo, Japan) under the intravascular ultrasound guide ( Figure 2(f)). Then, the GuideLiner catheter was selectively inserted into the left coronary artery by anchoring it coaxially with the 1.5 mm balloon ( Figure 2(d)). A 1.5 mm semicompliance balloon in the lead, along with a mother-child system, including a 6-Fr AL-1 guide catheter and a GuideLiner catheter, was advanced close to the orifice of the coronary trunk ( Figure 2(c)). After extending the guide wire, we removed the diagnostic catheter and left only the guide wire ( Figure 2(b)). Therefore, we utilized a 5-Fr diagnostic AL-1 catheter to engage the coronary trunk and a 0.014-inch floppy guide wire (Sion blue®, Asahi Intecc, Aichi, Japan) was advanced into the distal portion of the LAD ( Figure 2(a)). We failed to engage the anomalous orifice of the coronary trunk by using a 6-Fr AL-1 guiding catheter (Boston Scientific, MN, USA). A 0.014-inch guide wire was advanced into the LAD in order to stabilize the diagnostic catheter.įigure 2 shows the results of the PCI performed on this patient. (c) Right anterior oblique view showing critical stenosis in the middle segment of the left anterior descending (LAD) artery. (b) Coronary artery angiography with 5-Fr Amplatz Left-1 (AL-1) diagnostic catheter showing the single coronary trunk. (a) Aortography with a pigtail catheter showing the anomalous origin of the coronary artery from the ascending aorta. The lesion in the middle of the LAD was considered the cause of the patient's symptoms then we planned to perform PCI via the transfemoral approach at a later date. The middle segment of the LAD was critically stenosed ( Figure 1(c)).
In order to stabilize the diagnostic catheter, a 0.014-inch guide wire was advanced into the septal branch of the left anterior descending (LAD) artery. A 5-Fr diagnostic Amplatz Left-1 (AL-1) catheter was engaged and demonstrated a single coronary trunk ( Figure 1(b)). Aortography showed that the coronary trunk was originating from the ascending aorta ( Figure 1(a)). He underwent coronary angiography via the transradial approach to estimate cardiac ischemia.Ĭoronary angiography showed no vessel arising from each coronary sinus. Echocardiography showed normal function and normal chamber size. An electrocardiogram obtained at rest showed sinus rhythm and no significant ST-T change. His serum creatinine level was 1.22 mg/dL and estimated glomerular filtration rate was 47 mL/min/1.73 m 2. The patient's coronary risk factors included hypertension and dyslipidemia. A 65-year-old male patient was admitted to our hospital complaining of chest oppression during light exertion.
